If you do not provide the beneficiary with notice that the services are excluded from coverage, you should append modifier -GY to the line item. Item or service statutorily excluded, does not meet the definition of any Medicare benefit or for non-Medicare insurers, and is not a contract benefit. The -GX modifier indicates you provided the notice to the beneficiary that the service was voluntary and likely not a covered service. A -GX modifier should be attached to the line item that is considered an excluded, non-covered service. Notice of liability issued, voluntary payer policy. There are three modifiers to consider when dealing with non-covered services: Services rendered to immediate relatives and members of the household are not eligible for payment. In this instance, you should document and code it as such. Cosmetic procedures are never covered unless there is a medically-necessary reason for a procedure. 
Medicare only covers three immunizations (influenza, pneumonia, and hepatitis B) as prophylactic physician services. These include preventive examinations represented by CPT codes 99381-99397. Some of the items and services Medicare doesn’t cover include Long-term care (also called custodial care) Most dental care Eye exams related to prescribing glasses Dentures Cosmetic surgery Acupuncture Hearing aids and exams for fitting them and Routine foot care.Ĭertain services are never considered for payment by Medicare. Other categories of services Medicare does not pay include bundled services and services for which another entity, such as workers’ compensation, are primarily responsible (often referred to as “coordination of benefits”). 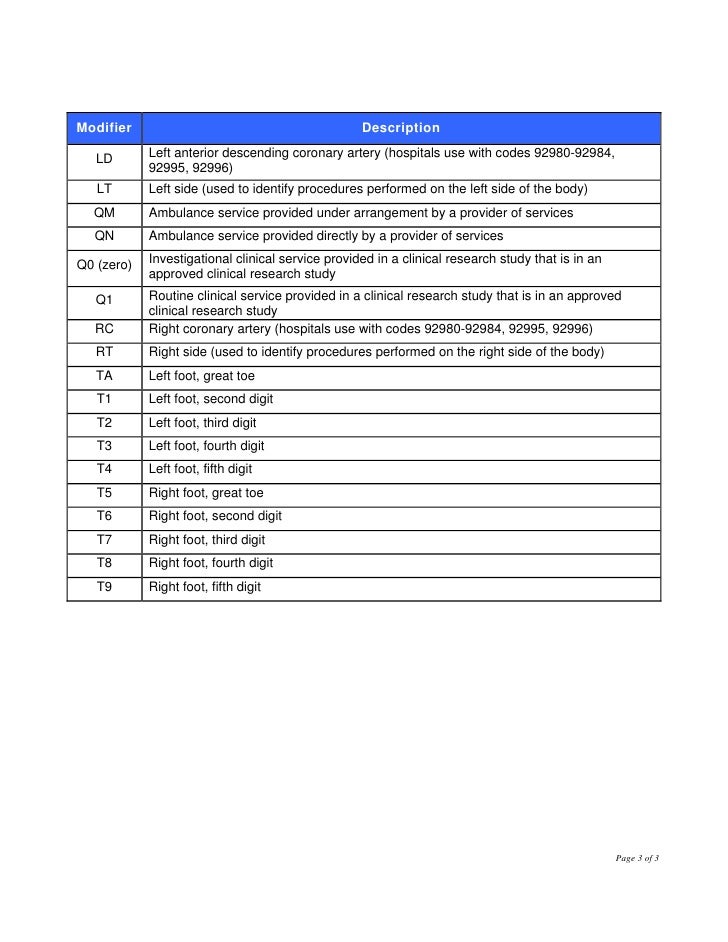
Understanding these rules and how to use them in your practice increases the likelihood of getting paid for the services your patients need, even if Medicare doesn’t cover them. In some instances, Medicare rules allow a physician to bill the patient for services in these categories. Services not deemed medically reasonable and necessary.There are two main categories of services which a physician may not be paid by Medicare: These modifiers are not required by Medicare but do allow for clean claims processing and billing to the patient. Pre-emptive communication through a voluntary ABN can prevent negative patient perceptions of your practice and facilitate collections. While not required, the ABN provides an opportunity to communicate with the patient that Medicare does not cover the service and the patient will be responsible for paying for the service. Non-covered services do not require an ABN since the services are never covered under Medicare. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
